Runners Knee
A common cause of Anterior Knee Pain.
What is patella femoral syndrome?
This term is used to describe pain around the patella(kneecap). The patella femoral joint is the joint between the femur (thigh bone) and the patella. The biomechanics of this joint are important to consider when explaining patella femoral pain syndrome. The patella sits in a groove on the femur (the trochlear groove). As the knee moves the patella glides across the front of the knee in this shallow groove. The patella moves up and down, tilts and rotates and there are therefore various points of contact between the patella and the femur.
The movement or tracking of the patella during movement of the knee requires a precisely timed, specific pattern of muscle contraction to ensure optimum movement of the patella through the trochlear groove. Improper patella tracking is thought to be one of the causes of patella femoral pain syndrome as are misdirected mechanical forces on the joint.
Maltracking of the patella occurs when the patella no longer remains centred in the trochlear groove, and develops an abnormal set of biomechanics resulting in increased pressure on the patellar articular (joint) surface. This causes abnormalities within the articular cartilage, chronic inflammation and pain.
What factors contribute to patella femoral syndrome?
There are a number of factors that predispose an individua lto patella femoral syndrome and these can be considered as causes that need to be addressed:
1. Abnormal biomechanics
1. Excessive pronation. Femoral anteversion – this is an internal rotation of the femur (thigh bone) and presents with the patellae (kneecaps) pointing inwards at each other. Increased Q angle – Q angle is the angle between the line of pull of the quadriceps muscles and the line of the patella tendon. Women often have wider hips than men and therefore their femurs (thigh bones) come to the patellae at a greater angle. This increases Q angle and can increase the chance that the patella is not properly aligned. Small patellae, which are highly positioned.
2. Muscle Imbalance
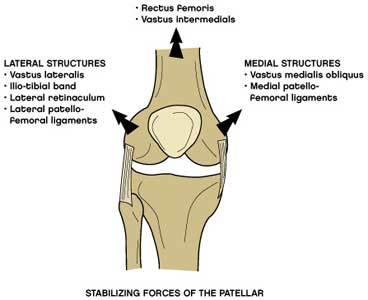
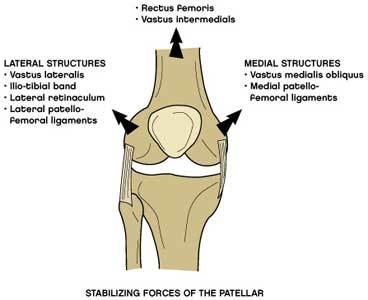
Tightness of the lateral structures of the patella femoral joint (as explained below). Weakness of the quadriceps muscles particularly the vastus medialis obliquus muscle (as explained below). Tightness of the calf and hamstring muscles. The stabilizing forces on the patella femoral joint are shownbelow:
The lateral (outside) stabilizing structures of the patella femoral joint are stronger than the medial (inside) structures so any imbalance in forces will tend to cause the patella to move more laterally and thus abnormally. Tightness of the lateral structures and weakness of the medial structures, particularly vastusmedialis obliquus will cause the patella to move more laterally in this way.
Symptoms:
- Pain around the patella, which may be non-specific.
- Pain aggravated by; running (especially downhill), stairs or any weight-bearing activity requiring repeated knee flexion (bending).
- Pain after prolonged periods of sitting.
- May experience clicking of the knee or crepitus (grinding) under the patella.
- May have tenderness on palpation of the patella.
- May have some swelling.
Treatment:
- Rest from aggravating activities.
- ICE therapy – apply ice to the knee for 10 – 15mins 2 – 3 times daily. Wrap the ice in a damp cloth and check the skin regularly.
- Use non-steroidal anti-inflammatory drugs (eg. Ibuprofen). Always consult your General Practitioner / Pharmacist for dosages etc…
- Quadriceps strengthening exercises – particularly focused on the vastus medialis obliquus muscle. One such exercise is detailed below:
Step downs:
Stand with one leg on a step. The foot of the leg on the stepshould be turned slightly outward. Gently squat down, ensuring that your knee is aligned over the 2ndtoe of the foot on the step. Push backup again and repeat. This exercise should be done in pain free range and as the muscle may fatigue quickly should be done in small numbers regularly through the day. Repeat on both legs.
Stretching of the lateral structures.
Stretch 1:
In sitting, with your legs outstraight in front, cross the leg to be stretched over the other, bending at the knee so that the foot moves towards the opposite hip. Pull the knee of the leg to be stretched towards the opposite shoulder using the opposite arm.
Stretching of the hamstrings, calfs and quadriceps. Massage Therapy – To release tightness in the lateral structures. Get someone to use their forearm and apply pressure to the outside of the thigh starting at the knee and sliding slowly towards the hip. You may also try using a rolling pin to self-treat. Strengthening of the gluteal muscles to control rotation at the hip. Ensure appropriate footwear. You may require motion control shoes or orthotics to control over pronation. Consult a Chartered physiotherapist who may use other forms of treatment including taping of the patella and electrotherapy. They will also be able to give you further more specific strengthening exercises and other advice. On full recovery from patella femoral pain syndrome you can decrease the risk of
reoccurrence by:
- A gradual increase in training intensity.
- Continuing appropriate stretches.
- Ensuring an adequate strengthening programme as part of your training to include specific work for the quadriceps and gluteals.
- Ensuring footwear remains correct.
Similar Posts:
- Runners Knee
- Iliotibial Band Syndrome
- What You Need To Know About Iliotibial Band Injuries
- What Are Shin Splints?
- What is Achilles Tendonitis
- What is Plantar Fasciitis